Understanding Scalp Psoriasis Symptoms: Key Signs, Effects, and When to Seek Care
Scalp psoriasis can look and feel different from routine dandruff, and knowing the key signs helps you decide when it is time to seek care. This overview explains how to recognize common symptoms, what they mean for your scalp and hair, where psoriasis may spread, and which triggers can worsen flares—so you can discuss options with a clinician in your area.
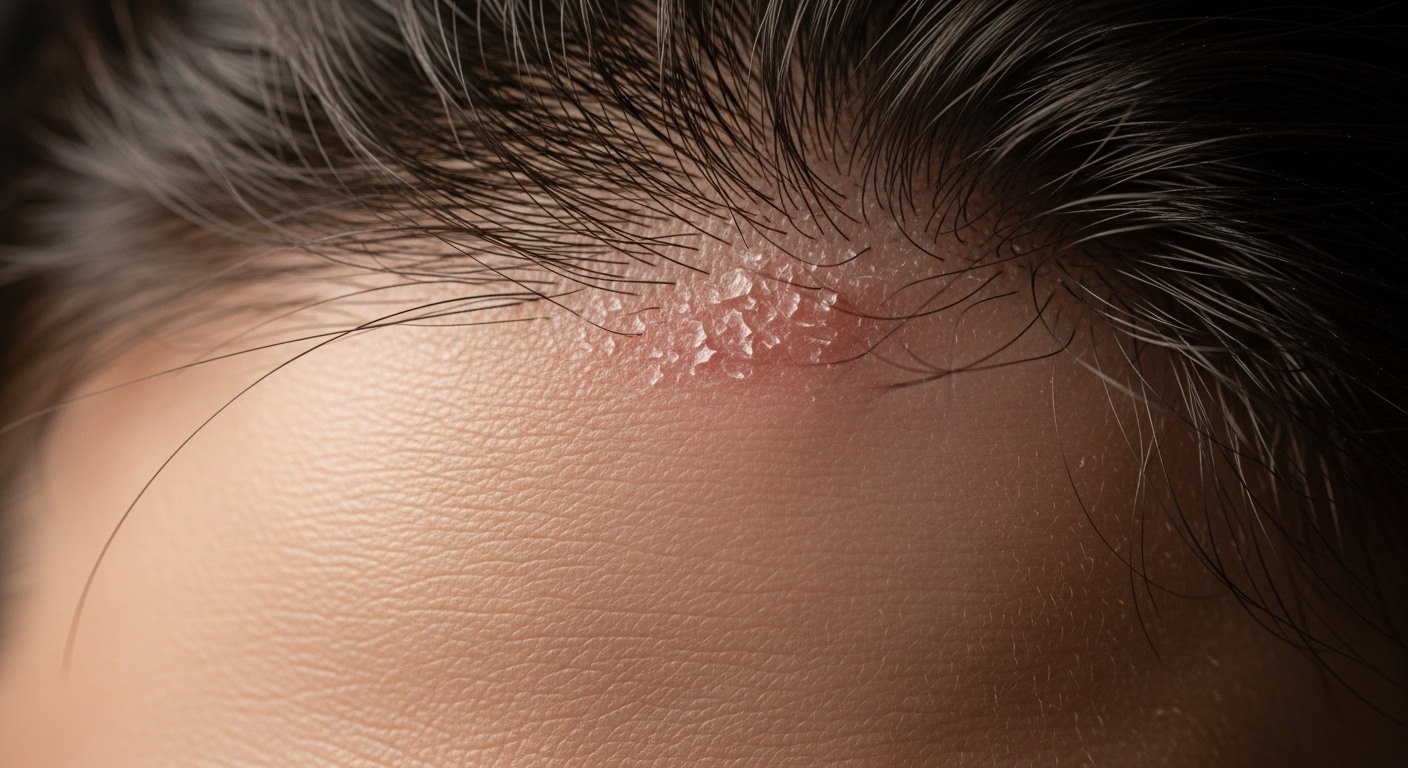
Scalp psoriasis is an immune-mediated skin condition that produces areas of inflamed skin covered by a build-up of thick, silvery scale. It is not contagious, and it can range from a few small patches to extensive plaques across the scalp. Because scaling and flakes are highly visible on dark clothing and hair, symptoms often affect daily comfort and confidence. Understanding how psoriasis presents on the scalp—and how it differs from dandruff or seborrheic dermatitis—can make conversations with a clinician more productive.
What do red patches and silvery scales show?
Scalp psoriasis typically appears as well-defined red or salmon-colored patches (plaques) topped by silvery-white scales. These plaques may feel raised, firm, and dry to the touch. Borders are often sharp, and removing scale can reveal pinpoint bleeding. Lesions may cluster in the crown, temples, or occiput and can vary from coin-sized to palm-sized. Unlike simple dandruff, patches are inflamed and may be tender, especially if scales are picked or scratched.
Itching, burning, and scalp discomfort explained
Itch is one of the most common and disruptive symptoms. Burning, stinging, or tightness can accompany active inflammation, especially during flares. Scratching may briefly relieve itch but can injure skin and trigger new plaques where the skin was irritated, a phenomenon known as the Koebner response. Nighttime itch can disturb sleep, and repeated scratching increases the risk of soreness or crusting. Gentle cleansing, avoiding harsh brushes, and reducing heat styling may help reduce discomfort between clinician visits.
Flaking, dandruff-like shedding, and effects on hair
Psoriatic scale tends to be thicker and more adherent than ordinary dandruff. When it loosens, flakes can be large and plate-like, creating dandruff-like shedding on clothing and shoulders. Hair itself is not permanently damaged by psoriasis, but temporary shedding can occur. This is most often due to inflammation around follicles, vigorous scratching, or frequent tight hairstyles that tug on hairs already loosened by scale. Using detangling techniques, avoiding picking at plaques, and choosing gentle, fragrance-free hair products can help limit breakage and visible shedding.
Spread to hairline, ears, and nails
Scalp psoriasis often extends a few millimeters beyond the hairline onto the forehead, nape, or behind the ears, where skin is thin and creases trap scale. Ear involvement can include the outer ear or ear canal, where buildup may feel like blockage and worsen itching. Although nails grow from a different structure, nail changes—including pitting (small indents), ridging, white or yellow discoloration, and lifting from the nail bed—can occur in people with scalp involvement. Some people also notice plaques on elbows, knees, or the lower back. Recognizing these related signs helps provide a fuller picture when you seek local services.
Severity, triggers, and when to seek care
Severity can be thought of in terms of area covered, thickness of plaques, and the degree of itch, pain, or sleep disruption. Common triggers include stress, cold or dry weather, skin injury (cuts, tight braids, chemical irritants), and some infections. Certain medications—such as lithium, some beta-blockers, and antimalarials—can exacerbate psoriasis for some individuals. Consider seeing a clinician in your area if you have: persistent itching or burning that affects sleep or daily life; bleeding, cracking, or painful plaques; widespread scaling or rapid worsening; suspected ear canal involvement; nail changes interfering with function; signs of infection (increasing warmth, pus, fever); or uncertainty about the diagnosis, especially if symptoms began suddenly in a child or during pregnancy.
Distinguishing scalp psoriasis from look-alikes
Several conditions can mimic scalp psoriasis. Seborrheic dermatitis typically produces greasy, yellowish scale on pink skin and is often itchier in the eyebrows, sides of the nose, or chest. Tinea capitis (a fungal infection) can cause patchy hair loss and broken hairs. Contact dermatitis flares where hair products touch the skin and improves when the trigger is removed. Because treatments differ, a clinician may inspect your skin, ask about triggers and family history, and, if needed, perform gentle scale removal or tests to confirm the diagnosis.
Symptom impact and self-care considerations
Beyond physical symptoms, visible flaking and redness can affect mood and social comfort. Managing stress with sleep hygiene, physical activity, or relaxation techniques may help reduce flares for some people. Wash the scalp regularly with lukewarm water, pat dry instead of rubbing, and avoid picking at adherent plaques to reduce soreness and the risk of new lesions forming in irritated areas. If you use headwear, choose breathable fabrics. When trying over-the-counter options in your area, follow label directions carefully and stop if you notice irritation.
Conclusion Recognizing visible signs such as red plaques and silvery scale, tracking discomfort like itching or burning, and noting spread to the hairline, ears, or nails can clarify whether symptoms align with scalp psoriasis. Understanding typical triggers and the difference from look-alike conditions supports timely conversations with a clinician and helps reduce the day-to-day burden of flaking and scalp discomfort.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.




